2026-04-01 東北大学
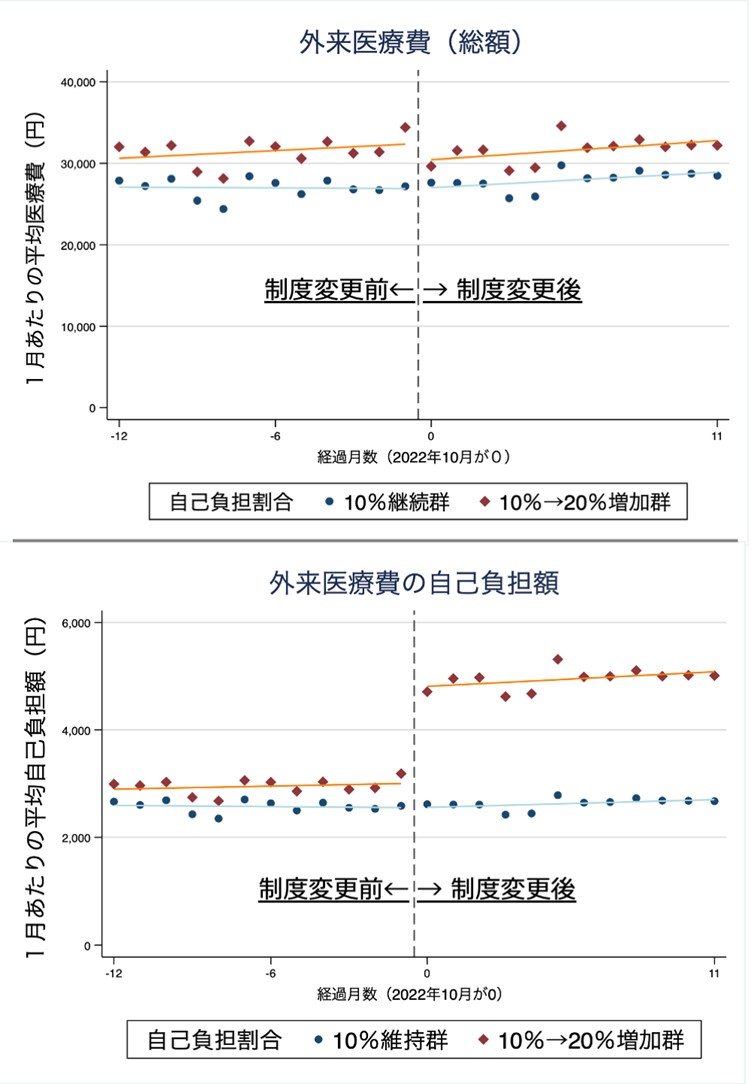
図1. 自己負担割合引き上げ前後の1ヶ月あたりの総外来医療費(上段)と自己負担額の推移
*補足:比較のために制度変更前後で自己負担割合が10%のままであった後期高齢者を対照群として、図内に示しています。
<関連情報>
- https://www.tohoku.ac.jp/japanese/2026/04/press20260401-02-cost.html
- https://www.tohoku.ac.jp/japanese/newimg/pressimg/tohokuuniv-press20260401_02_cost.pdf
- https://link.springer.com/article/10.1186/s12913-026-14387-4
高齢者の外来医療費に対する自己負担率引き上げの影響:日本の自己負担制度改革に関する準実験的研究 Impacts of cost-sharing rate increment on the expenditure of outpatient care among older adults: quasi-experimental study of cost-sharing reform in Japan
Taro Kusama,Yudai Tamada,Manami Hoshi-Harada,Ken Osaka & Kenji Takeuchi
BMC Health Services Research Published:19 March 2026
DOI:https://doi.org/10.1186/s12913-026-14387-4 Unedited version
Abstract
Background
Ensuring equitable access to healthcare under universal health coverage is critical; however, the financial sustainability of public health insurance systems faces challenges in aging societies. The present study aimed to evaluate the impact of the 2022 cost-sharing reform to increase coinsurance rate on outpatient care utilization among older adults with relatively high income, and to estimate the price elasticity of demand for outpatient care in response to the cost-sharing increase.
Methods
Employing a quasi-experimental design, this cohort study treats the 2022 cost-sharing reform as a natural intervention. Data were drawn from medical claims covering individuals aged ≥75 years enrolled in the Latter-Stage Elderly Healthcare System in several Japanese prefectures. Participants included 22,013 individuals in the intervention group (coinsurance increased from 10% to 20%) and 104,461 in the control group (coinsurance remained at 10%), observed from October 1, 2021, to September 30, 2023. An increase in coinsurance rate from 10% to 20% implemented on October 1, 2022, was treated as an exposure variable. Monthly total expenditures on outpatient care—physician visits, prescriptions, and dental visits—served as primary outcomes. Changes in total expenditure post-reform were assessed using controlled interrupted time series analysis, fitting a log-gamma regression model. Relative ratios (RRs) and 95% confidence intervals were estimated, and price elasticities were calculated using the change in out-of-pocket expenditures as denominators.
Results
Average total expenditures for overall outpatient care among the intervention group pre- and post-reform were ¥31,468 (SD=¥53,072) and ¥31,607 (SD=¥57,897) per month, respectively. Following the reform, expenditures significantly decreased for physician visits (RR=0.92 [0.90–0.94]) and prescriptions (RR=0.95 [0.93–0.97]) immediately after the reform, while dental visit expenditures did not significantly change (RR=0.97 [0.93–1.01]). Calculated price elasticities were highly inelastic (−0.137, −0.079, and −0.047 for physician visits, prescriptions, and dental visits, respectively).
Conclusions
These findings suggest that increasing the coinsurance rate led to modest short-term reductions in outpatient care expenditures among older adults with relatively high incomes. Outpatient care demand was largely inelastic to price changes, supporting the potential for income-based cost-sharing policies to enhance the financial sustainability of public health insurance systems with limited reduction in access.