2026-03-11 東京大学
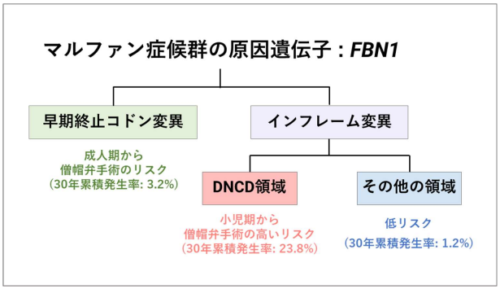
概要図
<関連情報>
- https://www.h.u-tokyo.ac.jp/participants/research/saishinkenkyu/20260311.html
- https://www.h.u-tokyo.ac.jp/participants/research/saishinkenkyu/__icsFiles/afieldfile/2026/03/12/release_20260311_1.pdf
- https://www.sciencedirect.com/science/article/abs/pii/S073510972600238X
マルファン症候群における僧帽弁手術の遺伝子型に基づくリスク層別化 Genotype-Guided Risk Stratification of Mitral Valve Surgery in Marfan Syndrome
Yuki Kawashima MD, Norifumi Takeda MD, PhD, Akiharu Omori MD, Yoshitsugu Nogimori MD, PhD, Kazuhiro Shiraga MD, Hitomi Masuda MD, Hiroki Yagi MD, PhD, Yuki Taniguchi MD, PhD, Haruo Yamauchi MD, PhD , Minoru Ono MD, PhD, Ryo Inuzuka MD, PhD
Journal of the American College of Cardiology Available online: 11 March 2026
DOI:https://doi.org/10.1016/j.jacc.2026.01.059
Abstract
Background
Although genotype-based risk stratification for aortic disease has been extensively studied in Marfan syndrome (MFS), mitral valve disease has received less attention despite being a major cardiovascular complication requiring surgery in up to 16% of cases.
Objectives
The authors aimed to evaluate genotype-specific differences in mitral valve disease progression and surgical intervention to inform precision medicine approaches in MFS.
Methods
This retrospective cohort study included 437 MFS patients with pathogenic FBN1 variants (2006-2024). Variants were classified by molecular mechanism (premature termination codon [PTC] variants vs in-frame variants [IFVs]) and genomic location. Time-to-event cause-specific analysis assessed genotype-specific risks for mitral valve surgery.
Results
Among 437 patients, 206 (47.1%) had PTC variants and 231 (52.9%) IFVs. Mitral valve surgery was performed in 38 patients (8.7%) at median age of 25.0 years. Among IFVs, those within the DNCD region (Dominant Negative variants affecting Cysteine residues and in-frame Deletions; exons 26-37 and 44-50) showed markedly higher 30-year cumulative incidence of mitral valve surgery (23.8% [95% CI: 11.7%-35.9%] vs 1.24% [95% CI: 0.0%-2.96%] in other IFVs and 3.20% [95% CI: 0.66%-5.77%] in PTC variants). IFVs within the DNCD region showed the earliest onset of mitral valve surgery in childhood/adolescence, whereas PTC variants demonstrated delayed risk beginning around age 30 years. Cox analysis confirmed IFVs within the DNCD region had highest risk of mitral valve surgery for patients aged ≤30 years (HR: 7.83 vs PTC variants; 95% CI: 3.14-19.57; P < 0.001) with robust discrimination (C-index = 0.725).
Conclusions
IFVs within the DNCD region confer the highest risk for mitral valve surgery with distinct age-dependent patterns. These findings enable genotype-guided risk stratification with age-specific surveillance protocols, potentially transforming clinical management in MFS.