2026-04-13 京都大学
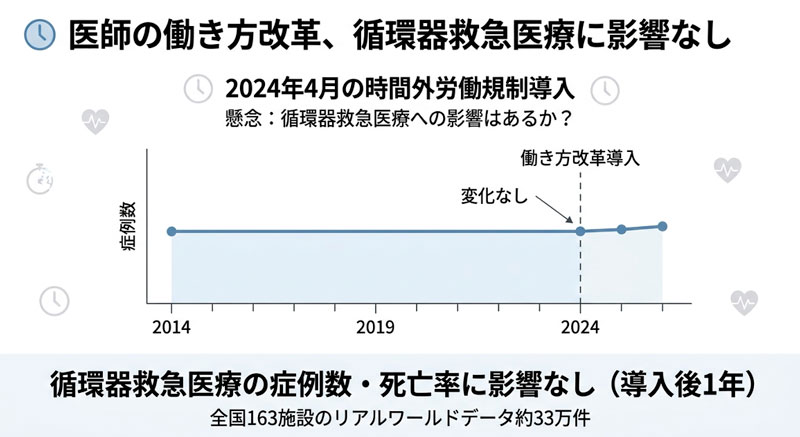
医師働き方改革導入前後の循環器救急医療の概念図(作成:森下哲司、Google Flow(Google Labs, 2026年3月利用))
<関連情報>
- https://www.kyoto-u.ac.jp/ja/research-news/2026-04-13-1
- ttps://www.kyoto-u.ac.jp/sites/default/files/2026-04/web_2604_Takada-aeaa7b944bd05e2d0ef54b738faebacd.pdf
- https://link.springer.com/article/10.1007/s12928-026-01283-1
日本の2024年医師働き方改革が心血管再血行再建に与えた初期影響 Early impact of Japan’s 2024 physician work hour reform on cardiovascular revascularization: a multi-center interrupted time series analysis using a National-Level DPC database
Tetsuji Morishita,Daisuke Takada,Hisashi Itoshima,Maki Mima,Susumu Kunisawa & Yuichi Imanaka
Cardiovascular Intervention and TherapeuticsPublished:12 April 2026
DOI:https://doi.org/10.1007/s12928-026-01283-1
Abstract
Japan introduced nationwide physician work-hour limits in April 2024. Because cardiovascular emergencies require continuous in-hospital availability, concerns existed that restricting duty hours could reduce access to revascularization or worsen clinical outcomes. We performed a nationwide retrospective interrupted time series analysis using weekly data from 163 acute-care hospitals participating in the Quality Indicator/Improvement Project database. Adult patients undergoing percutaneous coronary intervention (PCI) or coronary artery bypass grafting (CABG) for ischemic cardiovascular disease between 2014 and 2024 were included. Weekly procedure counts were modeled using segmented Poisson regression with adjustment for secular and seasonal trends. In-hospital mortality was evaluated as a secondary outcome. Subgroup analyses assessed weekend/holiday presentations, primary PCI achieving door-to-balloon time < 90 min, and institutional work-hour designation. A total of 329,659 revascularization procedures were analyzed. After April 2024, no significant immediate change and no significant change in slope were observed for weekly emergent PCI (level Risk Ratio (RR) = 0.97, 95% confidence interval (CI) 0.92–1.02), emergent CABG (RR = 0.83, 95% CI 0.58–1.17), elective PCI, or total PCI/CABG. Subgroup analyses showed consistent results, with stable weekly counts among weekend/holiday emergent PCI and primary PCI with door-to-balloon time < 90 min, and in hospitals under both Level A and Level B work-hour standards. In-hospital mortality for emergent PCI (RR = 1.11, 95% CI 0.91–1.36), elective PCI, and emergent CABG also showed no significant change. Early implementation of Japan’s physician work-hour reform was not associated with reductions in revascularization activity or increases in short-term mortality.