2023-07-21 カロリンスカ研究所(KI)
◆この技術は動脈硬化の早期予測に役立ち、心筋梗塞や脳卒中などの重篤な症状の予防に寄与する可能性があります。さらに、今後は動脈硬化の発症に関連する遺伝子やメカニズムの研究、他の血管部位に対する応用にも取り組む予定です。
<関連情報>
- https://news.ki.se/ai-and-precision-medicine-may-discover-risk-of-cardiovascular-disease
- https://academic.oup.com/cardiovascres/advance-article/doi/10.1093/cvr/cvad106/7226279
頸動脈潜在性アテローム性動脈硬化症のエンドタイプを特定する機械学習ベースのアプローチ A machine learning based approach to identify carotid subclinical atherosclerosis endotypes
Qiao Sen Chen, Otto Bergman, Louise Ziegler, Damiano Baldassarre, Fabrizio Veglia, Elena Tremoli, Rona J Strawbridge, Antonio Gallo, Matteo Pirro, Andries J Smit,Sudhir Kurl, Kai Savonen, Lars Lind, Per Eriksson, Bruna Gigante
Cardiovascular Research Published::21 July 2023
DOI:https://doi.org/10.1093/cvr/cvad106
Abstract
Aims
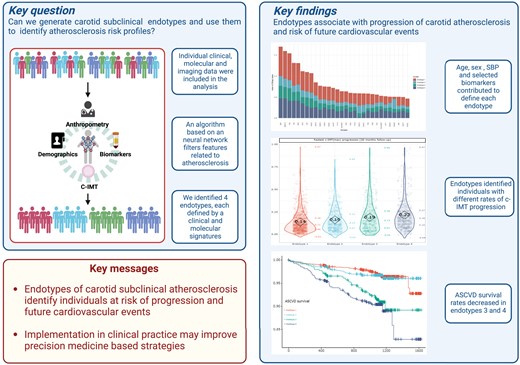
To define endotypes of carotid subclinical atherosclerosis.
Methods and results
We integrated demographic, clinical, and molecular data (n = 124) with ultrasonographic carotid measurements from study participants in the IMPROVE cohort (n = 3340). We applied a neural network algorithm and hierarchical clustering to identify carotid atherosclerosis endotypes. A measure of carotid subclinical atherosclerosis, the c-IMTmean-max, was used to extract atherosclerosis-related features and SHapley Additive exPlanations (SHAP) to reveal endotypes. The association of endotypes with carotid ultrasonographic measurements at baseline, after 30 months, and with the 3-year atherosclerotic cardiovascular disease (ASCVD) risk was estimated by linear (β, SE) and Cox [hazard ratio (HR), 95% confidence interval (CI)] regression models. Crude estimates were adjusted by common cardiovascular risk factors, and baseline ultrasonographic measures. Improvement in ASCVD risk prediction was evaluated by C-statistic and by net reclassification improvement with reference to SCORE2, c-IMTmean-max, and presence of carotid plaques. An ensemble stacking model was used to predict endotypes in an independent validation cohort, the PIVUS (n = 1061). We identified four endotypes able to differentiate carotid atherosclerosis risk profiles from mild (endotype 1) to severe (endotype 4). SHAP identified endotype-shared variables (age, biological sex, and systolic blood pressure) and endotype-specific biomarkers. In the IMPROVE, as compared to endotype 1, endotype 4 associated with the thickest c-IMT at baseline (β, SE) 0.36 (0.014), the highest number of plaques 1.65 (0.075), the fastest c-IMT progression 0.06 (0.013), and the highest ASCVD risk (HR, 95% CI) (1.95, 1.18–3.23). Baseline and progression measures of carotid subclinical atherosclerosis and ASCVD risk were associated with the predicted endotypes in the PIVUS. Endotypes consistently improved measures of ASCVD risk discrimination and reclassification in both study populations.
Conclusions
We report four replicable subclinical carotid atherosclerosis—endotypes associated with progression of atherosclerosis and ASCVD risk in two independent populations. Our approach based on endotypes can be applied for precision medicine in ASCVD prevention.