2025-03-31 アメリカ国立衛生研究所(NIH)
<関連情報>
- https://www.nhlbi.nih.gov/news/2025/social-factors-help-explain-worse-cardiovascular-health-among-adults-rural-vs-urban
- https://jamanetwork.com/journals/jamacardiology/fullarticle/2832034
- https://www.sciencedirect.com/science/article/pii/S073510971935079X
米国農村部と都市部の成人における心血管の健康-ヘルスケア、ライフスタイル、社会的要因 Cardiovascular Health Among Rural and Urban US Adults—Healthcare, Lifestyle, and Social Factors
Michael Liu, MPhil; Lucas X. Marinacci, MD; Karen E. Joynt Maddox, MD, MPH; et al
JAMA Cardiology Published:March 31, 2025
DOI:10.1001/jamacardio.2025.0538
Key Points
Question How does the burden of cardiometabolic risk factors and cardiovascular diseases differ between rural and urban areas of the US, and do health care access, lifestyle factors, and social risk factors contribute to any rural-urban differences in cardiovascular health?
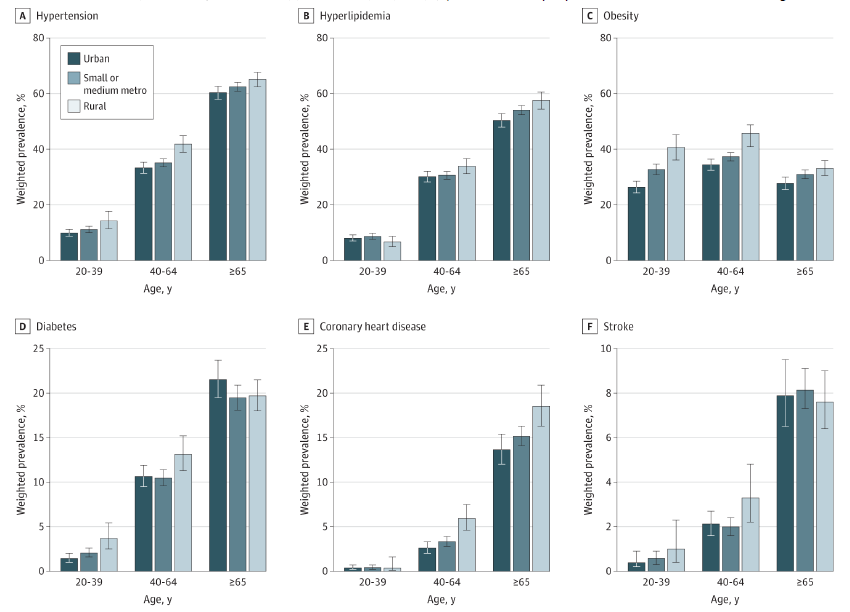
Findings In this national cross-sectional study of US adults, age-standardized rates of hypertension, hyperlipidemia, obesity, diabetes, and coronary heart disease were significantly higher in rural vs urban areas. Many rural-urban disparities in cardiovascular health were largest among young adults (aged 20-39 years) and almost entirely explained by social risk factors.
Meaning Efforts to improve socioeconomic conditions across the rural US may be important to close the rural-urban gap in cardiovascular health.
Abstract
Importance Improving cardiovascular health in rural areas is a national priority in the US. However, little is known about the current state of rural cardiovascular health and the underlying drivers of any rural-urban disparities.
Objective To compare rates of cardiometabolic risk factors and cardiovascular diseases between rural and urban US adults and to evaluate the extent to which health care access, lifestyle factors, and social risk factors contribute to any rural-urban differences.
Design, Setting, and Participants This nationally representative cross-sectional study analyzed data from US adults aged 20 years or older residing in rural vs urban areas using the 2022 National Health Interview Survey. Data were analyzed between August 2024 and February 2025.
Exposure County-level rurality.
Main Outcomes and Measures The primary outcomes were age-standardized rates of cardiometabolic risk factors (hypertension, hyperlipidemia, obesity, and diabetes) and cardiovascular diseases (coronary heart disease [CHD] and stroke).
Results The study population consisted of 27 172 adults, including 4256 adults (14.0%) residing in rural areas, 14 741 (54.8%) in small or medium metropolitan areas, and 8175 (31.2%) in urban areas. Mean (SD) participant age was 49.1 (17.8) years, and 4399 participants (50.8%) were female. Compared with their urban counterparts, rural adults were more likely to smoke, be insufficiently physically active, and have more social risk factors. Age-standardized rates of cardiometabolic risk factors were significantly higher in rural areas, including hypertension (37.1% vs 30.9%; rate ratio [RR], 1.20; 95% CI, 1.13-1.27), hyperlipidemia (29.3% vs 26.7%; RR, 1.10; 95% CI, 1.03-1.18), obesity (41.1% vs 30.0%; RR, 1.37; 95% CI, 1.27-1.47), and diabetes (11.2% vs 9.8%; RR, 1.15; 95% CI, 1.02-1.29). The same pattern was observed for CHD (6.7% vs 4.3%; RR, 1.58; 95% CI, 1.35-1.85), but no differences were observed for stroke. The magnitude of rural-urban disparities was largest among young adults (aged 20-39 years) for hypertension (RR, 1.44; 95% CI, 1.12-1.86), obesity (RR, 1.54; 95% CI, 1.34-1.77), and diabetes (RR, 2.59; 95% CI, 1.54-4.38). Rural-urban disparities in cardiovascular health were not meaningfully attenuated after adjustment for measures of health care access (insurance coverage, usual source of care, and recent health care utilization) and lifestyle factors (smoking and physical activity). However, accounting for social risk factors (poverty, education level, food insecurity, and home ownership) completely attenuated rural-urban disparities in hypertension (adjusted RR [aRR], 0.99; 95% CI, 0.93-1.06), diabetes (aRR, 1.02; 95% CI, 0.90-1.15), and CHD (aRR, 1.08; 95% CI, 0.91-1.29), but only partially attenuated disparities in obesity (aRR, 1.29; 95% CI, 1.20-1.39).
Conclusions and Relevance This national cross-sectional study found substantial rural-urban disparities in cardiometabolic risk factors and cardiovascular diseases, which were largest among younger adults and almost entirely explained by social risk factors. These findings suggest that efforts to improve socioeconomic conditions in rural communities may be critical to address the rural-urban gap in cardiovascular health.
社会経済格差と心血管疾患をつなぐストレス関連神経生物学的経路 Stress-Associated Neurobiological Pathway Linking Socioeconomic Disparities to Cardiovascular Disease
Ahmed Tawakol MD, Michael T. Osborne MD, Ying Wang MD, PhD, Basma Hammed MD, Brian Tung MS, Tomas Patrich BA, Blake Oberfeld BS, Amorina Ishai MD, Lisa M. Shin PhD, Matthias Nahrendorf MD, Erica T. Warner ScD, Jason Wasfy MD, Zahi A. Fayad PhD, Karestan Koenen PhD, Paul M Ridker MD, Roger K. Pitman MD, Katrina A. Armstrong MD
Journal of the American College of Cardiology Available online: 24 June 2019
DOI:https://doi.org/10.1016/j.jacc.2019.04.042
Central Illustration

Abstract
Background
Lower socioeconomic status (SES) associates with a higher risk of major adverse cardiac events (MACE) via mechanisms that are not well understood.
Objectives
Because psychosocial stress is more prevalent among those with low SES, this study tested the hypothesis that stress-associated neurobiological pathways involving up-regulated inflammation in part mediate the link between lower SES and MACE.
Methods
A total of 509 individuals, median age 55 years (interquartile range: 45 to 66 years), underwent clinically indicated whole-body 18F-fluorodeoxyglucose positron emission tomography/computed tomography imaging and met pre-defined inclusion criteria, including absence of known cardiovascular disease or active cancer. Baseline hematopoietic tissue activity, arterial inflammation, and in a subset of 289, resting amygdalar metabolism (a measure of stress-associated neural activity) were quantified using validated 18F-fluorodeoxyglucose positron emission tomography/computed tomography methods. SES was captured by neighborhood SES factors (e.g., median household income and crime). MACE within 5 years of imaging was adjudicated.
Results
Over a median 4.0 years, 40 individuals experienced MACE. Baseline income inversely associated with amygdalar activity (standardized β: -0.157 [95% confidence interval (CI): -0.266 to -0.041]; p = 0.007) and arterial inflammation (β: -0.10 [95% CI: -0.18 to -0.14]; p = 0.022). Further, income associated with subsequent MACE (standardized hazard ratio: 0.67 [95% CI: 0.47 to 0.96]; p = 0.029) after multivariable adjustments. Mediation analysis demonstrated that the path of: ↓ neighborhood income to ↑ amygdalar activity to ↑ bone marrow activity to ↑ arterial inflammation to ↑ MACE was significant (β: -0.01 [95% CI: -0.06 to -0.001]; p < 0.05).
Conclusions
Lower SES: 1) associates with higher amygdalar activity; and 2) independently predicts MACE via a serial pathway that includes higher amygdalar activity, bone marrow activity, and arterial inflammation. These findings illuminate a stress-associated neurobiological mechanism by which SES disparities may potentiate adverse health outcomes.