2026-04-02 国立循環器病研究センター
<関連情報>
- https://www.ncvc.go.jp/hospital/topics/topics_37047/
- https://www.ahajournals.org/doi/10.1161/SVIN.125.002024
発症後24時間以降の急性虚血性脳卒中に対する血管内治療:全国レジストリに基づく分析 Endovascular Therapy for Acute Ischemic Stroke Beyond 24 Hours After Onset: A Nationwide Registry-Based Analysis
Ryoma Inui, MD; Kanta Tanaka, MD, PhD; Kazunori Toyoda, MD, PhD; Sohei Yoshimura, MD, PhD; Kaori Miwa, MD, PhD; Tomohide Yoshie, MD, PhD; Junji Miyazaki, PhD; … ; Japan Stroke Data Bank Investigators
Stroke: Vascular and Interventional Neurology
DOI:https://doi.org/10.1161/SVIN.125.002024
Abstract
BACKGROUND:
This study aimed to evaluate the real-world status of endovascular therapy for acute ischemic stroke >24 hours after onset.
METHODS:
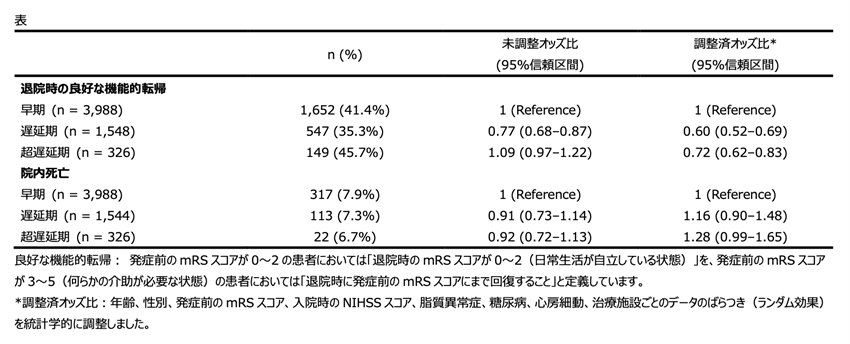
From the data set of Japan Stroke Data Bank, a nationwide, multicenter prospective registry of stroke within 7 days of onset, patients with acute ischemic stroke who underwent endovascular therapy from 2016 through 2021 were included. Patients were categorized into 3 groups according to time from onset to hospital arrival: early (<4.5 hours), late (4.5–24 hours), and very late (>24 hours). The primary outcome was a favorable functional status defined as a modified Rankin Scale (mRS) score of 0 to 2 at discharge for patients with a prestroke mRS score of 0 to 2, and return to prestroke mRS score at discharge for patients with a prestroke mRS score of 3 to 5.
RESULTS:
A total of 5862 patients were included (median age, 78 years; 42.7% women; median National Institutes of Health Stroke Scale score, 17; 83.8% with prestroke mRS score, 0–2), with 3988 in the early group, 1548 in the late group, and 326 in the very late group. The very late group was younger, had lower National Institutes of Health Stroke Scale scores, and a higher proportion of large artery atherosclerosis. The favorable functional status was achieved in 41.4%, 35.3%, and 45.7% of the early, late, and very late groups, respectively. In multivariable logistic analyses, both the late (adjusted odds ratio, 0.60 [95% CI, 0.52–0.69]) and very late (adjusted odds ratio, 0.72 [95% CI, 0.62–0.83]) groups showed lower odds of achieving a favorable functional status compared with the early group. When stratified by National Institutes of Health Stroke Scale score, achievement of the favorable functional status was less frequent in the late and very late groups, in that order, compared with the early group, particularly when the National Institutes of Health Stroke Scale score exceeded ≈10.
CONCLUSIONS:
In this nationwide registry, patients undergoing endovascular therapy >24 hours showed distinct clinical profiles, with crude outcomes comparable to patients treated in earlier time windows. These findings provide important context for the design and validation of randomized trials.