2026-03-24 東北大学
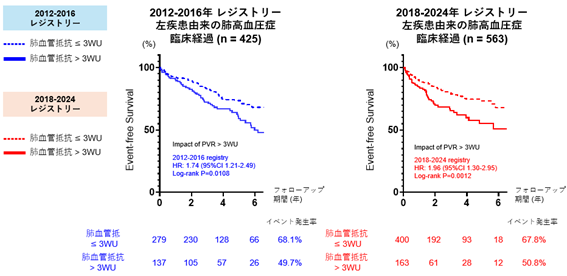
Group 2 PH症例では肺血管抵抗値が予後不良因子となる
<関連情報>
- https://www.tohoku.ac.jp/japanese/2026/03/press20260324-01-SiRIUS.html
- https://www.tohoku.ac.jp/japanese/newimg/pressimg/tohokuuniv-press20260324_web01_SiRIUS.pdf
- https://www.ahajournals.org/doi/10.1161/JAHA.125.045155
グループ2肺高血圧症における肺血管抵抗上昇の予後への影響:日本の多施設レジストリからの知見 Prognostic Impact of Elevated Pulmonary Vascular Resistance in Group 2 Pulmonary Hypertension: Insights From a Japanese Multicenter Registry
Taijyu Satoh, MD, PhD , Koichiro Sugimura, MD, PhD , Yoshihiro Fukumoto, MD, PhD , Kohtaro Abe, MD, PhD , Yoshihiro Dohi, MD, PhD , Kaoru Dohi, MD, PhD, Yu Taniguchi, MD, PhD ,…, Japan PH Registry Network Group 2 PH
Journal of American Heart Association Published: 20 March 2026
DOI:https://doi.org/10.1161/JAHA.125.045155
Abstract
Background
Group 2 pulmonary hypertension (PH), defined as PH caused due to left heart disease, remains a challenging condition. However, its prognostic impact and implications for emerging therapies are unclear. We aimed to evaluate the real‐world relationship between pulmonary vascular resistance (PVR) and prognosis in Group 2 PH and assess the efficacy of emerging therapies.
Methods
Two prospective registries supported by Japanese PH societies were analyzed: a current (2018–2024; n=563) and a previous (2012–2016; n=425) registry. The composite end points were hospitalization for heart failure, all‐cause death, ventricular assist device implantation, or cardiac transplantation.
Results
Stratified analyses using propensity score–matched data demonstrated a significant association between PVR >3 Wood units and prognosis in patients with Group 2 PH (6‐year event‐free rates, PVR >3 Wood units versus PVR ≦3 Wood units, previous registry: 72.9% versus 61.4%; current registry: 75.2% versus 55.4%). Consistent patterns were observed in both heart failure with reduced ejection fraction and heart failure with preserved ejection fraction subgroups. The use of SGLT2 (sodium‐glucose cotransporter‐2) inhibitors in the current registry was associated with improved outcomes in patients with elevated PVR, showing event‐free rates of 73.8% versus 35.5% in those without treatment. Among multivariate analyses including major treatment options, SGLT2 inhibitor treatment exhibited significant associations with improvement of composite end points.
Conclusions
Elevated PVR (>3 Wood units) identified a high‐risk subset of patients with Group 2 PH. The association between the use of SGLT2 inhibitors and better outcomes suggests a potential therapeutic role that warrants further investigation through controlled studies.