COVID-19感染症が重症化するほど、免疫系の活性化に必要な樹状細胞などの免疫細胞の回復が遅くなることが分かっています。LiUの研究者が研究で示した。COVID-19の重症化から6ヵ月後でも、数種類の免疫細胞に悪影響が見られる。 The more severe the COVID-19 infection, the slower the recovery of immune cells, such as the dendritic cells, which are necessary for the activation of the immune system. This is shown by researchers at LiU in a new study. Six months after severe COVID-19, a negative impact on several types of immune cells can still be seen.
2023-01-19 スウェーデン・リンショーピング大学
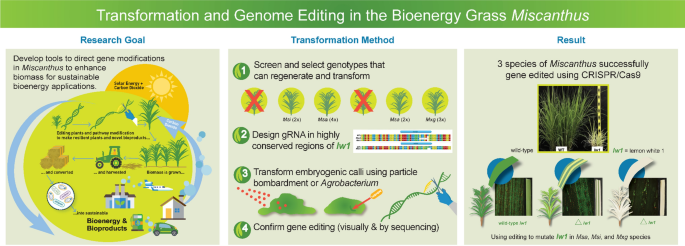
◆私たちの免疫系には、自然免疫系と適応免疫系の2つの部分があります。今回の研究では、自然免疫系を詳しく調べました。自然免疫系は、身体が特異的な免疫防御を組織化するために必要なものです。パンデミックの初期にSARS-CoV-2のような新しいウイルスに初めて遭遇したとき、免疫系はそれを検知しなければならない。そのためには、樹状細胞と呼ばれる一群の細胞が必要である。樹状細胞はT細胞を活性化し、SARS-CoV-2に感染した細胞を殺し、B細胞を活性化し、ウイルスを中和する抗体を作ることができます。したがって、樹状細胞は自然免疫系と適応免疫系をつなぐ重要な役割を担っているのです。同じ患者グループを対象とした以前の研究では、研究グループはT細胞への悪影響があることを発見しています。
◆研究者らは、ノルショーピングのVrinnevi病院に入院しているCOVID-19患者21人と、16人の健常者からなる対照群の血液サンプルを調査した。血液サンプルは4回に分けて採取され、最初は患者が入院したとき、最後は6~8ヵ月後に採取された。研究者らは、スペクトルフローサイトメトリーを用いて、さまざまなタイプの免疫細胞とその機能を同定した。
◆研究者らは、研究の中で、疾患の重症度と樹状細胞への影響との間に関連性を見いだした。体内の炎症過程で急速に増加するCRP(C反応性タンパク質)のレベルが高いほど、樹状細胞の回復が遅かったのです。また、CRPが体内で新しい樹状細胞を形成する能力を低下させる可能性を示す研究もあり、これが回復の遅さを説明する可能性もある。
◆「このことから得られる結論は、SARS-CoV-2ウイルスが暴走してCRP値を高くするのを防ぐために、抗ウイルス剤を感染のできるだけ早い段階で投与し、炎症を抑えるべきであるということです」とマリー・ラーソン氏は言う。
◆研究者たちは、組織に最も多く存在するもう一つの重要な種類の細胞、単球も調べた。この細胞は、何か異物や危険なものを感知すると、他の免疫細胞を引きつける信号を発し、炎症プロセスを引き起こす。その結果、6ヵ月後の患者さんでは、さまざまな種類の単球の分布が、健康な対照群とは異なることがわかりました。研究チームは、単球の変化は、体内、特に肺が重度の感染症から回復しつつあることを反映していると考えている。
<関連情報>
- https://liu.se/en/news-item/long-term-effects-on-the-innate-immune-system-following-covid-19
- https://www.frontiersin.org/articles/10.3389/fimmu.2022.1082912/full
COVID-19の入院後6ヶ月以上持続する単球および樹状細胞サブセットの大きな変化 Major alterations to monocyte and dendritic cell subsets lasting more than 6 months after hospitalization for COVID-19
Francis R. Hopkins, Melissa Govender, Cecilia Svanberg, Johan Nordgren, Hjalmar Waller, Åsa Nilsdotter-Augustinsson, Anna J. Henningsson, Marie Hagbom, Johanna Sjöwall, Sofia Nyström and Marie Larsson
Frontiers in Immunology Published:04 January 2023
DOI:https://doi.org/10.3389/fimmu.2022.1082912
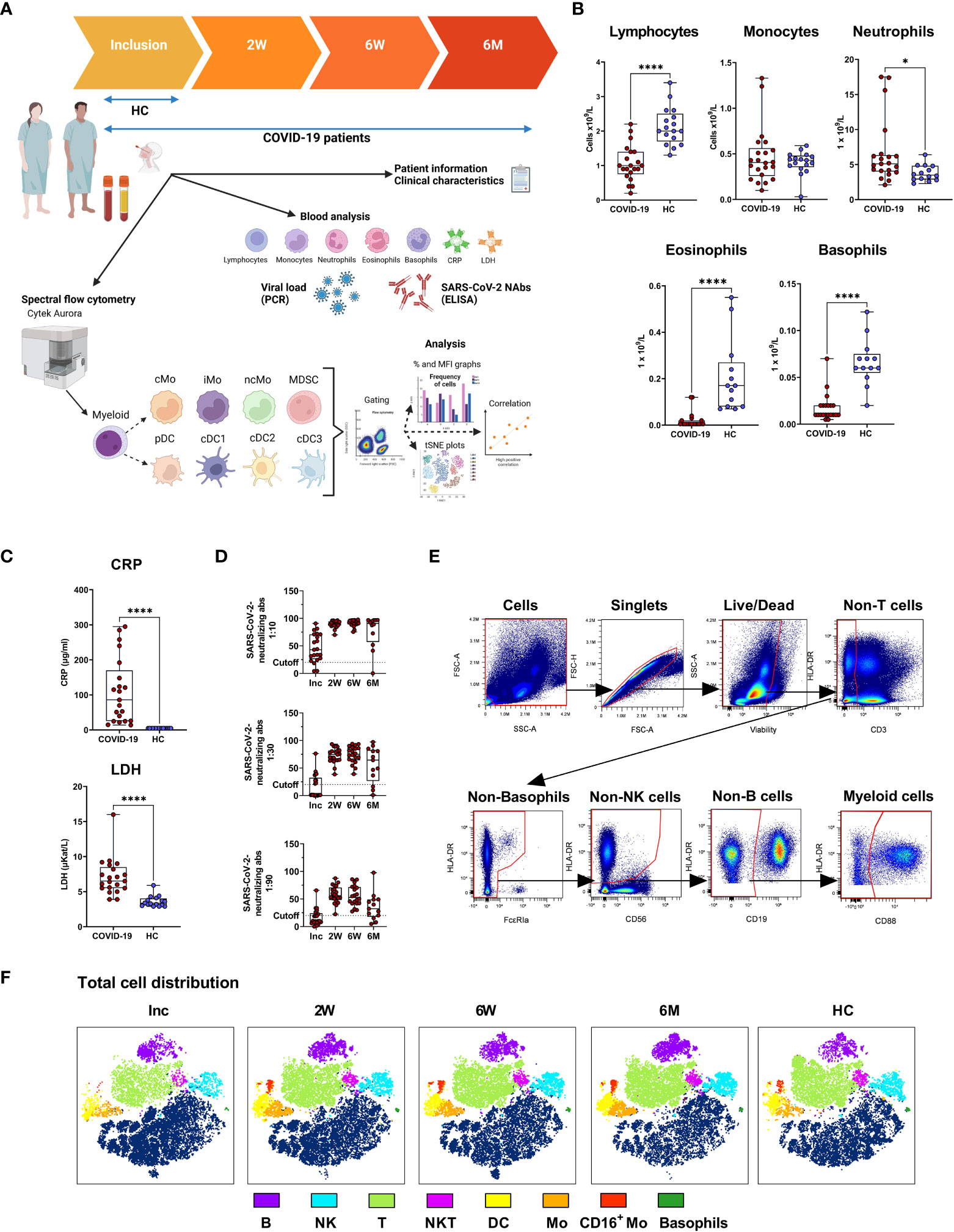
Introduction: After more than two years the Coronavirus disease-19 (COVID-19) pandemic continues to burden healthcare systems and economies worldwide, and it is evident that the effects on the immune system can persist for months post-infection. The activity of myeloid cells such as monocytes and dendritic cells (DC) is essential for correct mobilization of the innate and adaptive responses to a pathogen. Impaired levels and responses of monocytes and DC to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is likely to be a driving force behind the immune dysregulation that characterizes severe COVID-19.
Methods: Here, we followed a cohort of COVID-19 patients hospitalized during the early waves of the pandemic for 6-7 months. The levels and phenotypes of circulating monocyte and DC subsets were assessed to determine both the early and long-term effects of the SARS-CoV-2 infection.
Results: We found increased monocyte levels that persisted for 6-7 months, mostly attributed to elevated levels of classical monocytes. Myeloid derived suppressor cells were also elevated over this period. While most DC subsets recovered from an initial decrease, we found elevated levels of cDC2/cDC3 at the 6-7 month timepoint. Analysis of functional markers on monocytes and DC revealed sustained reduction in program death ligand 1 (PD-L1) expression but increased CD86 expression across almost all cell types examined. Finally, C-reactive protein (CRP) correlated positively to the levels of intermediate monocytes and negatively to the recovery of DC subsets.
Conclusion: By exploring the myeloid compartments, we show here that alterations in the immune landscape remain more than 6 months after severe COVID-19, which could be indicative of ongoing healing and/or persistence of viral antigens.