2026-03-02 九州大学
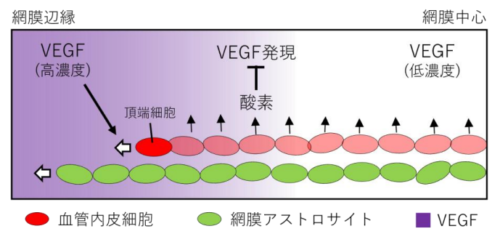
図1 数理モデル模式図血管伸長に先行して網膜アストロサイト(緑楕円)が拡がり、これを足場として頂端細胞(Tip cell)が運動した経路上に血管構造(赤楕円)が形成されると仮定した。この頂端細胞の運動は、血管から供給される酸素によって決定される VEGF 分布の勾配に誘引されると仮定した。
<関連情報>
- https://www.kyushu-u.ac.jp/ja/researches/view/1414
- https://www.kyushu-u.ac.jp/f/64973/26_0302_02.pdf
- https://tvst.arvojournals.org/article.aspx?articleid=2811550&resultClick=1
ヒト網膜中心窩無血管帯周辺の血管パターンの数理モデル化 Mathematical Modeling of Human Retinal Vascular Pattern Around the Foveal Avascular Zone
Kotaro Yoshimura; Kei Sugihara; Ichiro Maruko; Tomohiro Iida; Takashi Miura
Translational Vision Science & Technology Published:March 2026
DOI:https://doi.org/10.1167/tvst.15.3.1
Abstract
Purpose: Human retinas have unique anatomical structures called the macula and an associated characteristic vascular pattern. Despite its clinical importance, the mechanism underlying the human-specific vascular pattern remains unknown because of limitations in experimental approaches using primate samples. This study aimed to elucidate such vascular formation process.
Methods: We first examined the effects of four hypothetical factors contributing to foveal avascular zone (FAZ) formation: inhibitory molecule secretion, chemoattractant depletion, tissue deformation (towing), and tip cell migration restriction. None reproduced the features of the human retinal vascular structure. Next, we developed a mathematical model of human retinal vascular development by considering endothelial cells and astrocytes. We assumed that retinal vessels form via angiogenesis according to the gradient of vascular endothelial growth factor and that astrocytes dynamically expand while avoiding the fovea, providing scaffolds for angiogenesis.
Results: Our astrocyte-coupling model recapitulated various features of the human retinal vascular pattern, including a radially outward vascular pattern from the optic disc, inferior and superior temporal arcades, FAZ formation, a radially inward vascular pattern around FAZ, and a vertically facing pattern toward the horizontal vascular borderline in the temporal region of FAZ. Other models did not support the other four hypotheses.
Conclusions: Our model explained human-specific retinal vascular formation as the combination of angiogenesis and vascular growth restriction by retinal astrocytes. These results also suggest the importance of astrocyte dynamics, particularly their timing of spreading.
Translational Relevance: Our modeling framework can be extended to abnormal vascular patterns observed in diseases, including retinopathy of prematurity.

