2026-03-25 東京科学大学
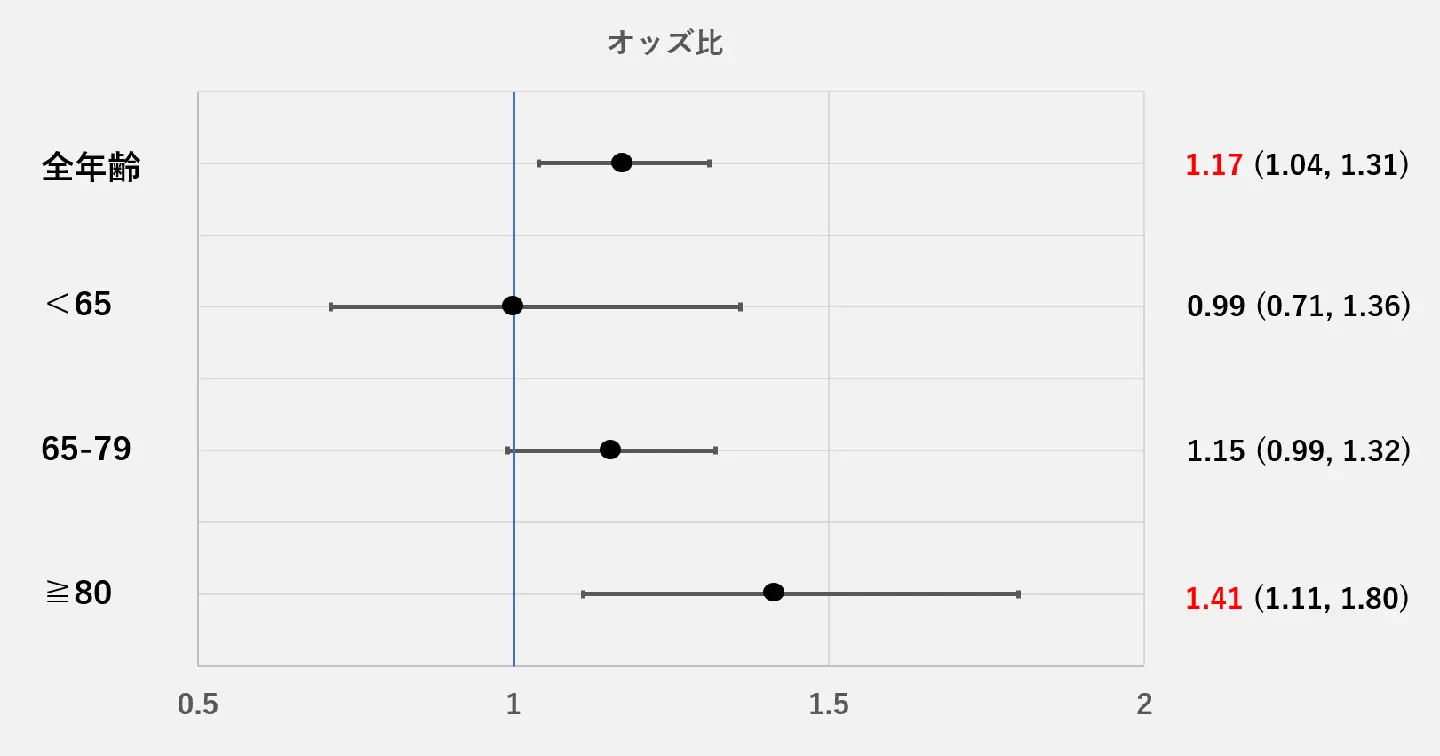
図1. 膵頭十二指腸切除術の術後90日以内死亡について、都会に対する地方のオッズ比
<関連情報>
- https://www.isct.ac.jp/ja/news/1c1jv5eusjts#top
- https://link.springer.com/article/10.1007/s00535-026-02357-w
膵頭十二指腸切除術後の院内死亡リスクにおける地域差:86,339人の患者を含む日本の全国データベースのデータを分析した横断研究 Regional differences for the risk of in-hospital mortality after pancreaticoduodenectomy: a cross-sectional study analyzing data from a Japanese nationwide database including 86,339 patients
Teruchika Koyama,Nobutoshi Nawa,Hisaaki Nishimura,Mariko Hanafusa,Keiichi Akahoshi,Hiroki Ueda,Kiyohide Fushimi & Takeo Fujiwara
Journal of Gastroenterology Published:02 March 2026
DOI:https://doi.org/10.1007/s00535-026-02357-w
Abstract
Background
Pancreaticoduodenectomy is the only curative treatment for pancreatic cancer, though it is an invasive procedure, with a high perioperative mortality rate, which may differ by region. The objectives of this study are to 1) investigate the risk of in-hospital mortality after pancreaticoduodenectomy in urban and rural hospitals, and 2) investigate its differences, stratified by age groups and hospital volume.
Methods
This study analyzed data from 86,339 patients who underwent pancreaticoduodenectomy from a Japanese nationwide database between 2010 and 2021. Hospitals were classified as urban if located in cities with ≥ 500,000 residents or in municipalities where ≥ 1.5% of residents commute to such cities, and all others were classified as rural. The primary outcome was in-hospital mortality within 90 days after pancreaticoduodenectomy. Logistic regression was applied.
Results
The risk for in-hospital mortality within 90 days after pancreaticoduodenectomy was significantly higher for patients in rural hospitals than those in urban hospitals (OR 1.17 [1.04–1.31]). Stratified analysis by age groups showed rural location was a significantly higher risk for patients ≧80 years old (OR 1.41 [1.11–1.80]), whereas there was no significant difference among patients aged ≤ 79 years. Stratified analysis by hospital volume and age groups showed that rural location was a significantly higher risk for patients ≧80 years old in low-volume hospitals (OR 1.43 [1.09–1.87]), whereas that was not significant for patients in high-volume hospitals.
Conclusions
The risk for in-hospital mortality was higher for rural hospitals than urban. Patients aged ≥ 80 years old in low-volume rural hospitals represented the highest-risk subgroup.