2026-04-27 統計数理研究所
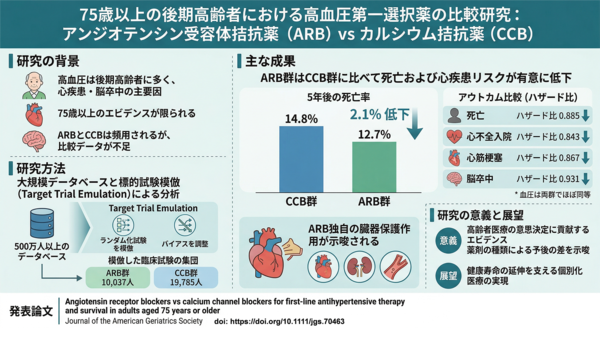
図1:75歳以上の後期高齢者における高血圧治療薬の比較研究。500万人以上の医療ビッグデータのデータベース分析より。
<関連情報>
- https://www.ism.ac.jp/ura/press/ISM2026-03.html
- https://agsjournals.onlinelibrary.wiley.com/doi/10.1111/jgs.70463
75歳以上の高齢者における高血圧治療薬の選択と生存への影響:アンジオテンシン受容体拮抗薬とカルシウム拮抗薬の比較研究 Angiotensin Receptor Blockers Versus Calcium Channel Blockers for First-Line Antihypertensive Therapy and Survival in Adults Aged 75 Years or Older
Hisashi Noma, Hiroshi Sunada, Taiki Sugimoto, Ken-Ei Sada, Futoshi Oda, Megumi Maeda, Haruhisa Fukuda
Journal of the American Geriatrics Society Published: 26 April 2026
DOI:https://doi.org/10.1111/jgs.70463
ABSTRACT
Background
Evidence guiding first-line antihypertensive drug choice in adults aged 75 years or older is limited, despite widespread use of angiotensin receptor blockers (ARBs) and calcium channel blockers (CCBs) in late older age.
Methods
We conducted a target trial emulation using a new-user design in a nationwide linked healthcare claims database in Japan. Adults aged ≥ 75 years who had no prescription of either drug class in the preceding 12 months and initiated an ARB (n = 10,037) or a CCB (n = 19,785) were followed from treatment initiation. The primary outcome was all-cause mortality; secondary outcomes included hospitalization for heart failure, myocardial infarction, stroke, and major adverse cardiovascular events (MACE). Intention-to-treat effects were estimated using inverse probability of treatment and censoring weighting with pooled logistic regression models.
Results
Among 29,822 patients, median follow-up was 4.0 years. During follow-up, 3487 deaths occurred. ARB therapy was associated with lower all-cause mortality than CCB therapy (hazard ratio [HR], 0.885; 95% CI, 0.823–0.951). The estimated 5-year risk of death was 12.7% for ARB users and 14.8% for CCB users (absolute risk difference, −2.1 percentage points; 95% CI, −3.1 to −1.0). ARB therapy was also associated with lower risks of heart failure hospitalization (HR, 0.843; 95% CI, 0.774–0.918), myocardial infarction (HR, 0.867; 95% CI, 0.795–0.945), stroke (HR, 0.931; 95% CI, 0.869–0.998), and MACE (HR, 0.889; 95% CI, 0.848–0.931). Associations were consistent across age subgroups, including adults aged ≥ 85 years.
Conclusion
In adults aged 75 years or older, ARB-based antihypertensive therapy was associated with lower risks of mortality and cardiovascular events compared with CCB-based therapy. These findings suggest that first-line antihypertensive drug choice may have prognostic implications in late older age.
Summary
- Key points○In this nationwide target trial emulation of 29,822 adults aged 75 years or older, angiotensin receptor blocker (ARB)-based therapy was associated with lower all-cause mortality compared with calcium channel blocker (CCB)-based therapy (HR 0.885; 5-year absolute risk difference −2.1 percentage points).
○ARB therapy was also associated with lower risks of heart failure hospitalization, myocardial infarction, and major adverse cardiovascular events, with consistent associations among adults aged 85 years or older.
○Achieved systolic and diastolic blood pressure levels were similar between treatment strategies, suggesting that differences in outcomes may not be explained solely by blood pressure control.
- Why does this paper matter?○Adults aged 75 years or older are frequently underrepresented in randomized trials of antihypertensive therapy, and ARBs and CCBs are often considered interchangeable first-line options in routine practice. In this large nationwide study, ARB-based therapy was associated with modest but clinically meaningful reductions in mortality and heart failure compared with CCB-based therapy. These findings suggest that antihypertensive drug choice in late older age may have prognostic implications beyond blood pressure lowering and may inform individualized prescribing decisions in geriatric care.