2026-03-23 国立循環器病研究センター
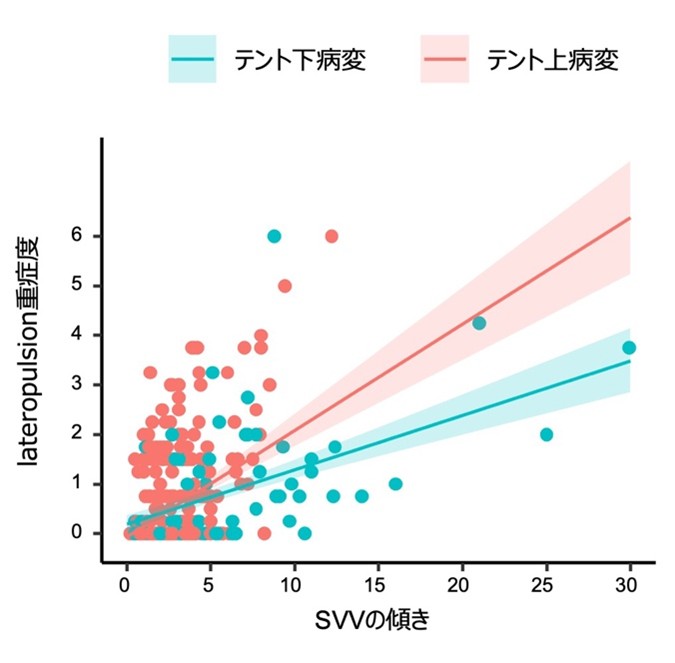
図1:責任病巣別のlateropulsionの重症度とSVVの関連性 出典:本論文を一部改変
<関連情報>
- https://www.ncvc.go.jp/hospital/topics/topics_36914/
- https://www.sciencedirect.com/science/article/abs/pii/S1877065726000035
テント上およびテント下脳卒中後の側方偏位と視覚的垂直傾斜:縦断的研究
Lateropulsion and visual vertical tilt after supra- and infratentorial stroke: a longitudinal study
Masatoshi Kamada, Chiaki Yokota, Shunsuke Murata, Katsuaki Shimano, Daishi Doda, Koichi Ito
Annals of Physical and Rehabilitation Medicine Available online: 19 March 2026
DOI:https://doi.org/10.1016/j.rehab.2026.102100
Dear Editor,
Lateropulsion is characterized by a disturbed perception of body orientation with respect to gravity and a disturbed representation of verticality [1−3]. This condition has been linked to disruptions in the ascending graviceptive pathway, which transmits gravitational information from the semicircular canals through the vestibular nuclei, brainstem, and thalamus to the vestibular cortex [4]. Because gravity sensing is not only mediated by the vestibular system, but also by the somatosensory system and vision [3,5], lateropulsion is not considered a simple vestibular dysfunction but rather an impairment of the multisensory
integration underlying verticality perception.
Subjective visual vertical (SVV) tilt is considered the most sensitive sign of a vestibular tone imbalance caused by the disruption of ascending graviceptive pathways [6]. After an infratentorial stroke with lateropulsion, SVV tilt is mainly due to ocular torsion [7,8], whereas in supratentorial stroke with lateropulsion, SVV tilt is thought to reflect disruption of the brain network involved in multisensory control of vertical perception [3,9]. To date, no large-scale series of studies have compared infratentorial and supratentorial strokes using SVV tilt in individuals with and without lateropulsion at the acute stroke phase. In addition, no longitudinal study has followed the course of verticalityperception impairment, as measured by SVV tilt, in individuals with lateropulsion. We hypothesized that after acute stroke onset, the change in SVV tilt with lateropulsion may differ between individuals with infratentorial and supratentorial stroke.
The aim of the present study was to: (1) compare SVV tilt between individuals with infratentorial stroke and individuals with supratentorial stroke at the acute phase with and without lateropulsion; and (2) follow the course of SVV tilt in individuals with lateropulsion, comparing those with infratentorial stroke to those with supratentorial stroke.
This was a single-center, retrospective observational study approved by the Ethics Committee of the National Cerebral and Cardiovascular Center (M28-063-18) and conducted in accordance with the Declaration of Helsinki. Informed consent was obtained from all participants. This study was registered with the UMIN Clinical Trials Registry (ID:UMIN000024655), operated by the University Hospital Medical Information Network in Japan (not WHO-labelled trial registration). The reporting follows STROBE guidelines (checklist in the appendix).
Individuals with acute stroke admitted within 48 h of stroke onset from August 2021 to July 2023 were recruited to our study. Stroke was diagnosed clinically by stroke physicians and confirmed by head MRI or CT on admission. Exclusion criteria were premorbid disability, unstable conditions, inability to complete the Scale for Contraversive Pushing (SCP) [10] assessment, inability to undergo SVV testing, multiple simultaneous strokes, or spatial neglect. Stroke lesions were categorized as supratentorial or infratentorial based on head MRI or CT findings.
The SCP and SVV tilt assessments were conducted on the initial day of walking rehabilitation. Participants with lateropulsion were followed up at least twice a week until discharge. Lateropulsion was assessed using the SCP, defined as an SCP score >0 (cutoff value = 0) [12]. Participants with upright posture scored 0 points on all SCP items. SVV testing was performed in a darkened room, with participants seated 50 cm from a display. A 30 cm white rod on the display at eye level was rotated continuously at five degrees per second, and participants signaled when they perceived the rod as vertical. Six trials (three clockwise and three
counterclockwise) were conducted at random, as in the previous study [13]. This number of trials represents the minimum required for robust SVV tilt estimation while minimizing patient burden. The SVV tilt was calculated as the mean signed deviation (in degrees), with positive values indicating ipsilesional tilt and negative values indicating contralesional tilt. A tilt >2.5° was defined as pathological SVV tilt [3,6].
Participants with spatial neglect were excluded if they demonstrated visual, tactile, auditory, spatial, or personal inattention or profound hemi-inattention, as assessed on the extinction and inattention item of the National Institutes of Health Stroke Scale [11]. After applying these criteria, individuals with complete SCP and SVV data were included as participants (Figure S1).
To investigate the association between lateropulsion and SVV tilt, we built logistic regression and linear regression models with lateropulsion