2026-03-27 国立循環器病研究センター
<関連情報>
- https://www.ncvc.go.jp/hospital/topics/topics_36952/
- https://www.ahajournals.org/doi/10.1161/JAHA.125.047724
高齢心房細動患者における抗凝固薬と抗血小板薬の併用療法の影響:ANAFIEサブ解析 Impact of Combined Anticoagulant and Antiplatelet Therapy in Older Patients With Atrial Fibrillation: ANAFIE Subanalysis
Naruhiko Kamogawa, MD; Kazunori Toyoda, MD, PhD; Takenori Yamaguchi, MD, PhD; Hiroshi Inoue, MD, PhD; Takeshi Yamashita, MD, PhD; Shinya Suzuki, MD, PhD; Hiroaki Kobayashi, MS; … ;ANAFIE investigators
Journal of the American Heart Association Published: 13 March 2026
DOI:https://doi.org/10.1161/JAHA.125.047724
Abstract
Background
We aimed to evaluate the impact of concomitant use of oral anticoagulants (OAC) and antiplatelet drugs (APD) on clinical outcomes compared with OAC monotherapy in patients aged ≥75 years with atrial fibrillation.
Methods
The ANAFIE (All Nippon AF [Atrial Fibrillation] in Elderly) Registry was a prospective multicenter observational study in Japan. This subanalysis included patients aged ≥75 years with nonvalvular atrial fibrillation receiving OAC. Patients were classified into OAC monotherapy and concomitant OAC+APD therapy groups. Clinical outcomes, including stroke/systemic embolism, major bleeding, and all‐cause mortality, were compared using Cox proportional hazards models. Within the OAC+APD group, outcomes were also compared between patients using direct OACs and those using warfarin.
Results
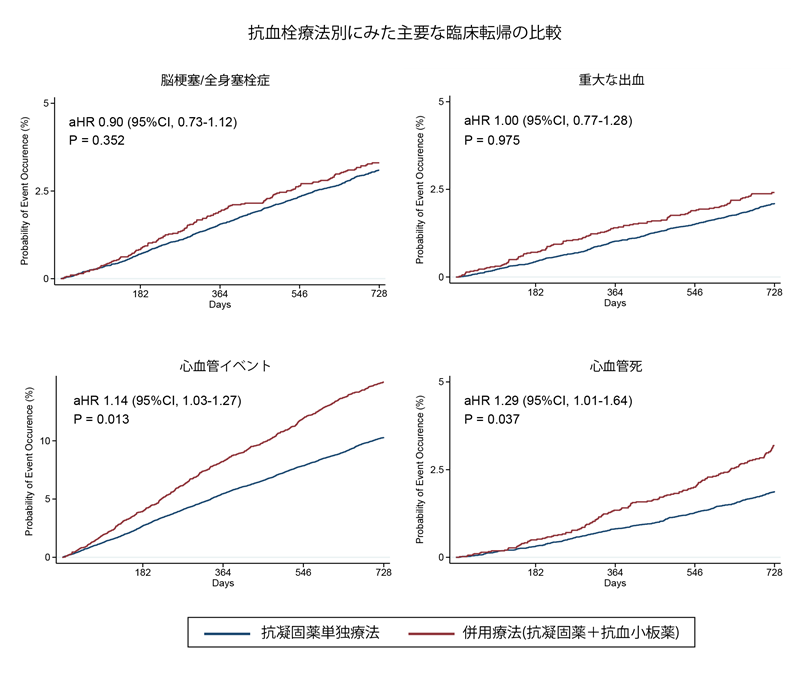
Among 29 818 patients (median age 81 years, 42.3% female), 4861 (16.3%) received OAC+APD therapy. This group had higher proportion of men, previous cerebrovascular disease, and previous myocardial infarction. The group showed increased risk of cardiovascular death [1.57 versus 0.94/100 person‐years, adjusted hazard ratio (aHR), 1.29 [95% CI, 1.01–1.64]. There were no significant differences in stroke/systemic embolism, major bleeding, or all‐cause mortality. Within the OAC+APD group, direct OAC use was associated with lower risks of stroke/systemic embolism (aHR, 0.55 [95% CI, 0.38–0.80]), intracranial hemorrhage (aHR, 0.52 [95% CI, 0.30–0.90]), and all‐cause mortality (aHR, 0.73 [95% CI, 0.58–0.91]) compared with warfarin.
Conclusions
In older patients with atrial fibrillation, OAC+APD therapy was associated with higher incidence of cardiovascular death than OAC monotherapy, without significant differences in other clinical outcomes. For patients requiring combination therapy, DOACs may be preferable to warfarin.