2026-03-31 東京科学大学
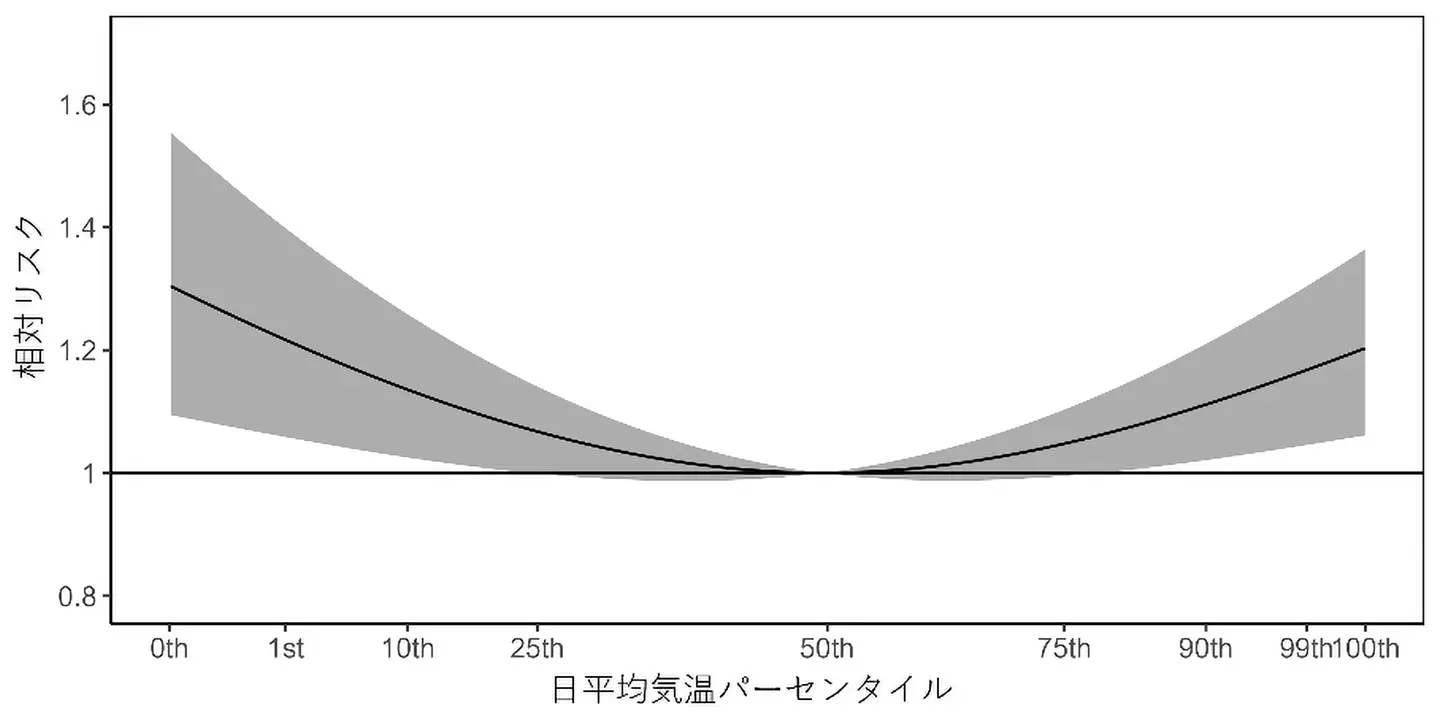
図1. 12日間のラグ効果を考慮した日平均気温パーセンタイル[用語3]と小児けいれんによる緊急入院のリスク
<関連情報>
外気温と小児けいれんによる入院:全国データセットを用いた時間層別分析 Ambient temperature and pediatric seizure hospitalization: a time-stratified analysis in a national dataset
Aomi Katagiri,Hisaaki Nishimura,Nobutoshi Nawa,Kiyohide Fushimi & Takeo Fujiwara
Pediatric Research Published:18 March 2026
DOI:https://doi.org/10.1038/s41390-026-04875-y
Abstract
Background
Nationwide studies investigating the association between pediatric seizures and both extreme heat and cold are lacking.
Methods
We identified emergency hospitalization for pediatric seizures aged 15 years old and younger, from 2011 to 2019 using a nationwide administrative database in Japan. A time-stratified case-crossover design with conditional quasi-Poisson regression was used to assess short-term associations between daily mean temperature and seizure-related hospitalizations across a lag period of up to 12 days. Daily mean temperature obtained from the Japan Meteorological Agency. Seizure-related hospitalizations based on International Classification of Diseases, Tenth Revision (ICD-10) codes G41.X and R56.X. Region-specific estimates were then pooled using a random-effects meta-analysis to calculate overall relative risks.
Results
A total of 116,353 cases were identified. After adjusting for relative humidity, the pooled relative risk (RR) at 99th percentile temperature (extreme heat) was 1.17 (95% CI: 1.05–1.30). For the 1st percentile temperatures (extreme cold), the pooled RR was 1.22 (95% CI: 1.06–1.40).
Conclusion
Both extreme cold and heat were associated with an increased risk of emergency hospitalization for pediatric seizures. These findings underscore the need for public health strategies for both hot and cold temperature extremes to protect the pediatric populations.
Impact
- This is the first nationwide study to show that both extreme cold and heat increase the risk of pediatric seizure–related hospitalizations, with effects peaking within 0–1 days.
- Using daily meteorological data and distributed lag non-linear models across Japan’s diverse climate zones, we provide robust evidence beyond prior local or single-facility studies.
- Findings highlight children’s physiological vulnerability to temperature extremes and emphasize adaptation strategies such as hydration, infection prevention, and minimizing exposure.
- Results inform clinical management and public health responses to pediatric seizure risks in the context of global climate change.