2023-09-18 カロリンスカ研究所(KI)
◆研究では、肥満の診断を受けたスウェーデンの170人以上の幼児を対象に、3つの治療条件(標準治療、親のサポートグループ、親のサポートグループにフォローアップ電話サポート)に分けて治療を行いました。
◆研究結果は、早期の肥満治療が子供たちの体重状態を改善し、代謝の健康も向上させることを示しました。この研究は、子供の肥満を早期に治療することが、後の年齢での治療よりも効果的であることを強調し、肥満手術を回避する可能性があると述べています。
<関連情報>
- https://news.ki.se/early-treatment-of-child-obesity-is-effective
- https://www.nature.com/articles/s41366-023-01373-7
肥満の幼児に対する治療の長期追跡調査:無作為化比較試験 A long-term follow-up of treatment for young children with obesity: a randomized controlled trial
Anna Ek,Markus Brissman,Karin Nordin,Karin Eli & Paulina Nowicka
International Journal of Obesity Published:18 September 2023
DOI:https://doi.org/10.1038/s41366-023-01373-7
Abstract
Background
Early childhood obesity interventions supporting parents have the largest effects on child weight status. However, long-term follow-ups are lacking.
Objective
To examine weight status 48 months after obesity treatment initiation for 4- to 6-year-olds.
Methods
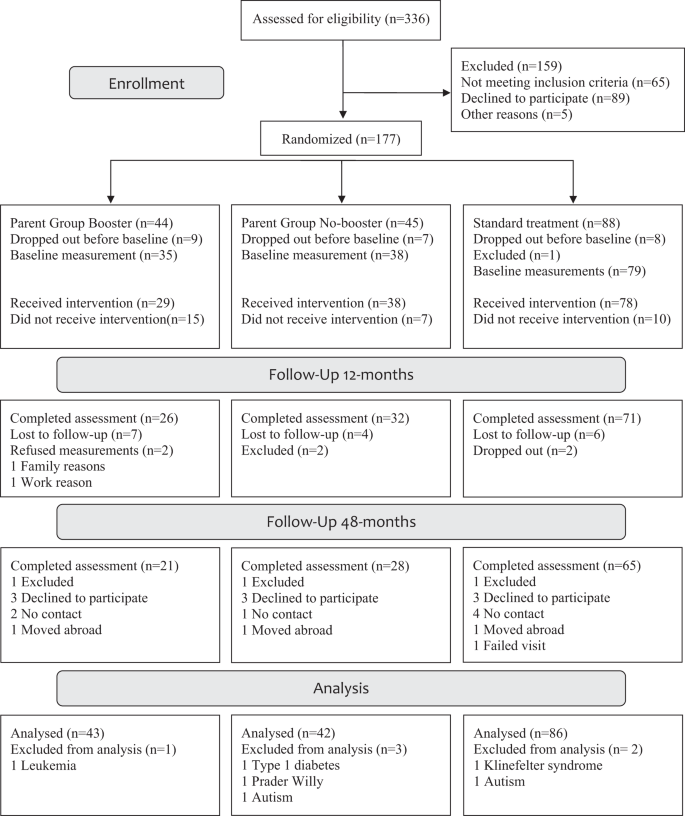
177 families were recruited to the More and Less study, a 12-month randomized controlled trial (RCT) conducted in Sweden (2012–2017); 6 children were excluded due to medical diagnoses. Thus, 171 families (non-Swedish origin 59%, university degree 40%) were eligible for this 48-month follow-up with modified intention-to-treat (n = 114 had 48-month data, n = 34 dropped out, n = 23 lost to follow-up). The RCT compared 3 treatment approaches: a 10-week parent support program (1.5 h/w) with follow-up booster sessions (PGB) or without (PGNB), and standard outpatient treatment (ST). Treatment effects on primary outcome (BMI-SDS) and secondary outcomes (BMI, %IOTF25 i.e., the distance, in percent, above the cut-off for overweight) were assessed. Clinically significant reduction of BMI-SDS (≥0.5) was assessed with risk ratio. Sociodemographic factors and attendance were examined by three-way interactions.
Results
After 48 months (mean 50 months, range 38–67 months) mean (95% CI) BMI-SDS was reduced in all groups: PGB -0.45 (-0.18 to -0.73, p < 0.001), PGNB -0.34 (-0.13 to -0.55, p < 0.001), ST -0.25 (-0.10 to -0.40, p < 0.001), no significant difference between groups. A clinically significant reduction of BMI-SDS ≥ 0.5 was obtained in 53.7% of PGB which was twice as likely compared to ST, 33.0%, RR 2.03 (1.27 to 3.27, p = 0.003), with no difference to PGNB, 46.6% (p = 0.113). %IOTF25 was unchanged from baseline for PGB 4.50 (-1.64 to 10.63), and significantly lower compared to ST 11.92 (8.40 to 15.44) (p = 0.043). Sociodemographics or attendance had no effect.
Conclusion
The intensive parent-support early childhood obesity intervention led to better weight status outcomes over time, though BMI-SDS alone did not reflect this. Further research should investigate how to assess weight changes in growing children.
Clinical trial registration
Clinicaltrials.gov, NCT01792531.