2026-04-13 国立成育医療研究センター
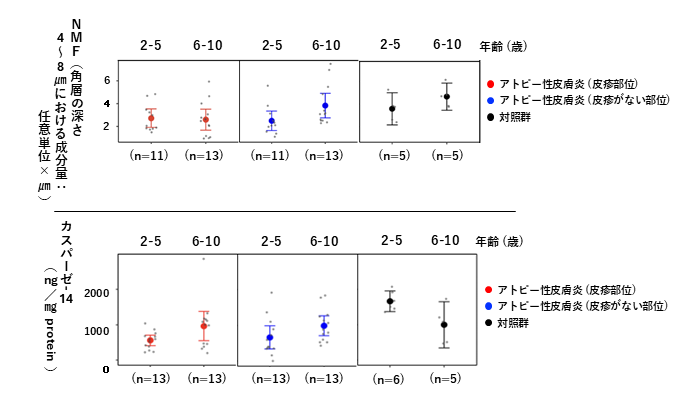
【図1:角層中の天然保湿因子(NMF)とカスパーゼ14の年齢群別の変化】
<関連情報>
小児アトピー性皮膚炎における天然保湿因子およびカスパーゼ-14の年齢依存的な減少 Age-dependent reductions in natural moisturizing factor and caspase-14 in paediatric atopic dermatitis
Risa Fukuda, Kyongsun Pak, Hazuki Yasuda, Tomoko Kawai, Kenichiro Hata, Naoko Mochimaru, Marie Takenouchi, Ryo Tanaka, Rena Hashimoto, Yuhki Ueda, Susumu Hashimoto, …
Journal of the European Academy of Dermatology and Venereology Published: 19 March 2026
DOI:https://doi.org/10.1111/jdv.70417
Dear Editor,
Impaired stratum corneum (SC) barrier function is central to the pathophysiology of atopic dermatitis (AD); however, the barrier characteristics of Asian children remain unclear.1 Natural moisturizing factors (NMFs), derived from filaggrin, contribute to SC hydration and integrity, and caspase-14 is a key protease involved in filaggrin degradation. Caspase-14 deficiency reduces NMF levels and impairs barrier function; adults with AD have shown reduced caspase-14 and NMF levels in lesional and non-lesional skin.2-4 Confocal Raman spectroscopy (CRS) enables non-invasive assessment of SC composition; however, the relationship between CRS-derived NMF and caspase-14 has not been investigated in paediatric AD.5 Therefore, we examined NMF and caspase-14 alterations in paediatric AD, with a particular focus on age-related differences because SC maturation undergoes a notable transition at around age 6.6
We enrolled 26 paediatric patients with mild-to-moderate AD and 11 healthy controls (aged 2–10 years). AD severity was assessed using the Eczema Area and Severity Index and national xerosis management guidelines.7 The controls had no allergic diseases or skin dryness. The SC components, including NMF levels, were assessed using CRS. Topical agents were withheld from the evaluation sites from the night before assessment. In patients with AD, lesional and non-lesional sites on the inner forearms were evaluated; the controls were assessed at a corresponding single site. Filaggrin and its degrading enzymes were collected by tape stripping and quantified using enzyme-linked immunosorbent assay. Exome sequencing was performed to identify FLG loss of function (LoF) variants. Statistical analyses involved non-parametric tests without adjustment for multiple comparisons because of the exploratory design.
Twenty-six patients with mild-to-moderate AD and 11 controls were analysed and stratified into two age groups: 2–5 and 6–10 years, and two patients with AD and one control carried FLG LoF variants (Table 1). NMF levels were lowest in lesional sites, followed by non-lesional sites, in the AD group, and were highest in the controls. In non-lesional sites, NMF levels were higher in children aged 6–10 years in both groups, whereas lesional sites exhibited persistently low NMF levels across all ages (Table 2, Figure 1a). The lowest levels of filaggrin and its degrading enzymes were in AD-lesional sites, followed by non-lesional sites, in both age groups. Caspase-14 levels were significantly decreased in lesional and non-lesional sites among children aged 2–5 years, whereas levels were comparable to those of controls in those aged 6–10 years (Figure 1b). Correlation analyses demonstrated negative correlations between NMF levels and filaggrin in lesional and non-lesional sites in patients with AD (Figure 1c).