2026-03-13 国立精神・神経医療研究センター
<関連情報>
- https://www.ncnp.go.jp/topics/detail.php?@uid=vADnBtza6kIhJ3F8
- https://www.cambridge.org/core/journals/psychological-medicine/article/exposurebased-cognitive-behavioral-therapy-delivered-by-assertive-community-treatment-teams-for-severe-mental-illness-with-symptoms-of-anxiety-a-cluster-randomized-controlled-trial/62E8BF580CAA43F59767A0D35A77A979
不安症状を伴う重度の精神疾患に対する、積極的地域治療チームによる曝露療法に基づく認知行動療法:クラスター無作為化比較試験 Exposure-based cognitive behavioral therapy delivered by assertive community treatment teams for severe mental illness with symptoms of anxiety: a cluster randomized controlled trial
Sayaka Sato,Asami Matsunaga,Makoto Ogawa,Masashi Mizuno,Akiko Kikuchi,Hiroaki Kumano,Sosei Yamaguchi andChiyo Fujii
Psychological Medicine Published:13 March 2026
DOI:https://doi.org/10.1017/S0033291726103365
Abstract
Background
Individuals with severe mental illnesses (SMIs) experience anxiety that impairs functioning and quality of life. This cluster randomized trial evaluated exposure-based cognitive behavioral therapy (ebCBT) integrated into assertive community treatment (ACT) teams to reduce anxiety.
Methods
Fifteen ACT teams were allocated to ebCBT + ACT (k = 8, n = 50) or ACT-only (k = 7, n = 43). The intervention followed four steps: situation identification, four-component analysis (behavior, cognition, emotion, physical symptoms), psychoeducation, and graded exposure. Staff received 50 h training and bimonthly supervision over 12 months. Co-primary outcomes were trait and social anxiety; secondary outcomes were psychiatric symptoms, functioning, quality of life, and recovery.
Results
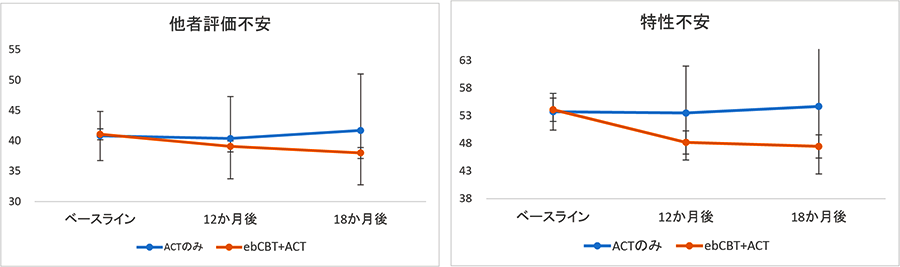
The ebCBT + ACT group showed significant improvements in State–Trait Anxiety Inventory–Trait scores at 12 months (AMD = −5.30, 95% CI = −8.71 to −1.90, p = 0.002, d = −0.64) and 18 months (AMD = −7.22, 95% CI = −12.1 to −2.34, p = 0.004, d = −0.60). Brief Fear of Negative Evaluation scores showed near-significant improvement at 18 months (AMD = −3.70, 95% CI = −7.44 to 0.04, p = 0.052, d = −0.40). Secondary outcomes, including global functioning, recovery, and quality of life, also improved. Cost-effectiveness analyses indicated favorable cost-effectiveness for anxiety outcomes.
Conclusions
Embedding ebCBT within ACT services may reduce anxiety-related fear and avoidance and enhance recovery-related outcomes in individuals with SMI. These findings support the feasibility and clinical value of integrating structured psychological interventions into intensive community-based outreach services.